Sleep disorders
Disrupted sleep patterns—from insomnia to excessive daytime sleepiness—erode cognitive performance and well-being, highlighting the need for tailored diagnostic and therapeutic strategies.
What are sleep disorders?
Sleep disorders are conditions that affect the quality, timing or quantity of sleep, leading to daytime symptoms such as fatigue, poor concentration, mood changes and reduced performance. Many are highly treatable with the right diagnosis and a personalised plan.


Conditions we commonly treat
-
Insomnia (difficulty falling or staying asleep)
-
Obstructive sleep apnoea (OSA) and snoring
-
Restless legs syndrome (RLS) and periodic limb movement disorder (PLMD)
-
REM sleep behaviour disorder (RBD) and other parasomnias (sleepwalking, night terrors)
-
Narcolepsy and idiopathic hypersomnia (excessive daytime sleepiness)
-
Circadian rhythm disorders (shift work, delayed sleep phase)
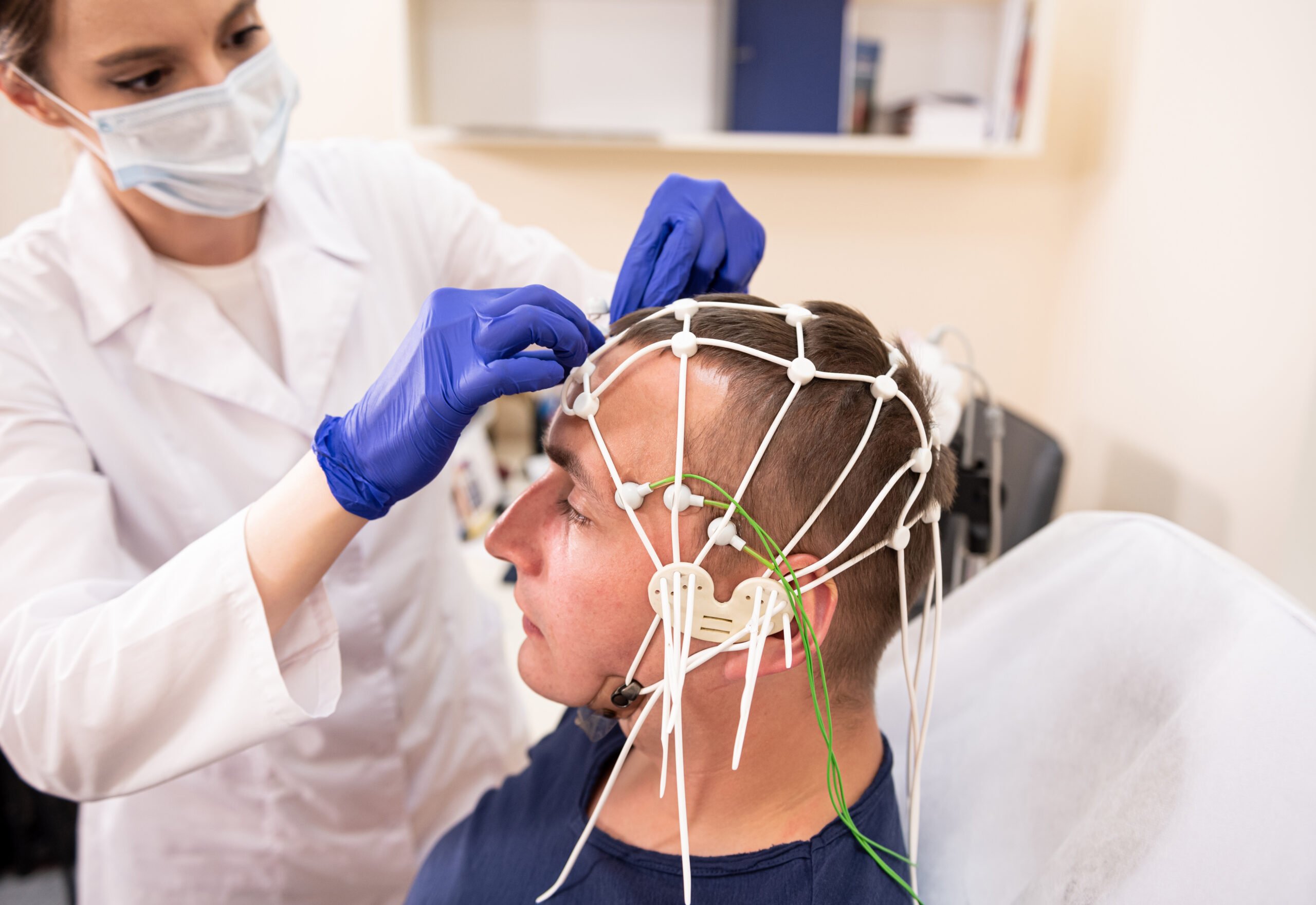
Diagnosis with neurophysiology expertise
-
Comprehensive sleep history and validated questionnaires (e.g., Epworth Sleepiness Scale)
-
Sleep diary/actigraphy to map patterns over 1–2 weeks
-
Overnight polysomnography (in-lab) or home sleep apnoea testing, as appropriate
-
Multiple Sleep Latency Test (MSLT)/Maintenance of Wakefulness Test (MWT) for suspected narcolepsy or hypersomnia
-
Video-EEG when events at night may be neurological (e.g., nocturnal seizures)
Dr FM’s background in neurophysiology ensures precise signal acquisition and interpretation, turning complex data into clear decisions.
Personalised treatment plans
-
Insomnia (CBT-I first): Stimulus control, sleep restriction, cognitive strategies, and targeted behavioural change—often more effective and longer-lasting than medication.
-
Sleep apnoea: Optimised CPAP/APAP therapy with careful mask fitting, adherence coaching and troubleshooting; consideration of positional therapy, weight management and mandibular advancement devices when suitable.
-
RLS/PLMD: Iron repletion when indicated, plus tailored pharmacological options and lifestyle adjustments.
-
RBD/parasomnias: Night-time safety measures, medication where appropriate and review for associated neurological conditions.
-
Narcolepsy/hypersomnia: Structured daytime scheduling, planned naps and wake-promoting therapies alongside driving and workplace guidance.
Living better, sleeping better
You’ll leave with a written plan covering sleep hygiene that actually works (consistent wake time, light exposure, caffeine/alcohol timing), technology and bedroom environment tips, and clear triggers for review.
FAQ
Will I need a sleep study?
Not always. Many cases improve with targeted behavioural therapy; studies are recommended when results will change management (e.g., suspected apnoea, narcolepsy or parasomnia)
Is medication the only option for insomnia?
No—CBT-I is first-line and often outperforms sleeping tablets in both effectiveness and durability.
If I start CPAP, is it forever?
CPAP controls apnoea when used; some people transition to alternative options if appropriate. Regular review ensures your plan fits your life.
What about pregnancy and MS?
Many people with MS have healthy pregnancies. Pre-conception counselling helps time DMTs and relapses safely.
BOOK YOUR CONSULTATION
Book a consultation with Dr Francesco Manfredonia (Dr FM) for clear diagnosis, compassionate care and a plan built around your life and goals.
